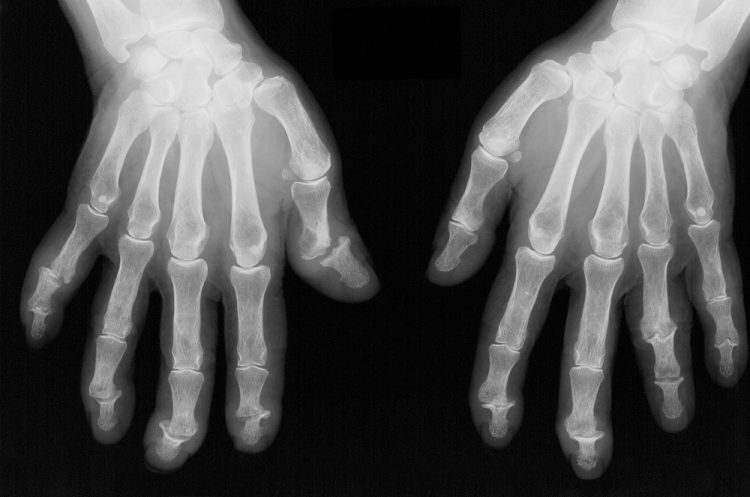
The burden of bone damage and trabecular bone loss at the
metacarpal heads is higher among patients with psoriatic arthritis (PsA)
compared with healthy controls, according to study results published in Osteoporosis International.1
Previous studies have showed that inflammatory PsA may cause
structural damage at the metacarpophalangeal joint, which makes the metacarpal
heads vulnerable to inflammation and bone loss in patients with PsA.2
The objective of this study was to compare bone structure and
microstructure in the metacarpal heads among patients with PsA and healthy
controls, and to identify demographic and clinical factors associated with bone
loss in patients with PsA.
Researchers evaluated data of 62 patients with PsA arthritis
and 62 age- and sex-matched healthy controls from the Rheumatology Clinic at
the Prince of Wales Hospital. All patients underwent a high-resolution
peripheral quantitative computed tomography exam of the second and third
metacarpal heads in the nondominant forearm. Researchers recorded the number
and size of bone erosions and enthesophytes at the second and third metacarpal
heads, along with volumetric bone mineral density (vBMD) and microstructure.
Correlation analysis and multivariable linear regression models were used to
determine the association of demographic and clinical characteristics with bone
loss in PsA.
Results of the study indicated that there were 85 erosions and 150 enthesophytes among patients with PsA, and 50 erosions and 80 enthesophytes among the healthy controls. At the second and third metacarpal heads, the mean number of erosion was similar among patients with PsA and healthy controls (1.4±1.2 vs 1.1±1.0; P =.110), though the total erosion volume per person was significantly greater among patients with PsA compared with healthy controls (5.2±6.0 mm3 vs 2.8±4.5 mm3; P =.003). The mean number, height, and volume of enthesophytes were also greater among patients with PsA than among the healthy controls at the second and third metacarpal heads.
Among patients with PsA, older age correlated with larger
erosion and enthesophyte volume. At the second and third metacarpal heads, compared
with healthy controls, older patients with PsA had significantly lower mean
vBMD (average vBMD, -6.9%; P =.007;
trabecular vBMD, -8.8%, P <.001;
peritrabecular vBMD, -7.7%; P =.001;
metatrabecular vBMD, -9.8%; P <.001),
average trabecular bone volume fraction (-8.8%; P <.001), and average trabecular bone thickness
(-8.1%; P =.003). Multivariable
linear regression analysis showed that older age and a higher C-reactive
protein level were independently associated with lower mean vBMD and trabecular
bone loss at the second and third metacarpal heads.
Study limitations included the fact that nearly one-fifth of patients with PsA with joint destruction were excluded from the analysis because of difficulties associated with analyzing severe joint deformity, and the cross-sectional design of the study that prevented a causal effect relationship from being established between bone damage and clinical characteristics.
“The burden of bone erosions, [enthesophytes], and trabecular bone loss is increased in patients [with] PsA compared with matched healthy controls. Patients [with] PsA had a predominant deterioration in trabecular microstructure in the metacarpal head, which was related to ongoing disease inflammation,” the researchers concluded.
References
1. Wu D, Griffith JF, Lam SHM, et al. Comparison of
bone structure and microstructure in the metacarpal heads between patients with
psoriatic arthritis and healthy controls: an HR-pQCT study [published
online January 14, 2020]. Osteoporos
Int. doi:10.1007/s00198-020-05298-z
2. Finzel S, Sahinbegovic E, Kocijan R, Engelke K,
Englbrecht M, Schett G. Inflammatory
bone spur formation in psoriatic arthritis is different from bone spur
formation in hand osteoarthritis. Arthritis
Rheum. 2014;66:2968-2975.