This was a cross sectional, monocentric study, conducted at the Luigi Sacco Hospital, Department of Biomedical and Clinical Science “L. Sacco”, University of Milan, Milan, Italy. The study title was “ScrEening the Retina in Patients wIth COVID-19″ (SERPICO-19). The study was approved by the local ethic committee (Protocol Number 2020/ST/088) and written informed consent was obtained from all participants. The study adhered to the tenants of the declaration of Helsinki.
2.3 Images analysis
All images were assessed by two retinal specialists (FZ and SP) to evaluate their quality. If the fundus details were not visible due to acquisition artifacts or media opacities in more than 2/4 photos the eye was not included in the analysis, if both eyes were graded “unreadable” the subject was excluded. For all included eyes the same retinal specialists assessed the images for the presence of any abnormal findings affecting the retina and/or the retinal vessels. In case of disagreement, a third senior retinal specialist (AI) was asked to evaluate the image.
]. In brief, retinal images were acquired and processed using the Automated Retinal Image analyzer (ARIA, V1-09-12-11), an opensource software developed on the MATLAB platform (MATLAB R2020a – update 1 (9.8.0.1359463)) [
].
,
].

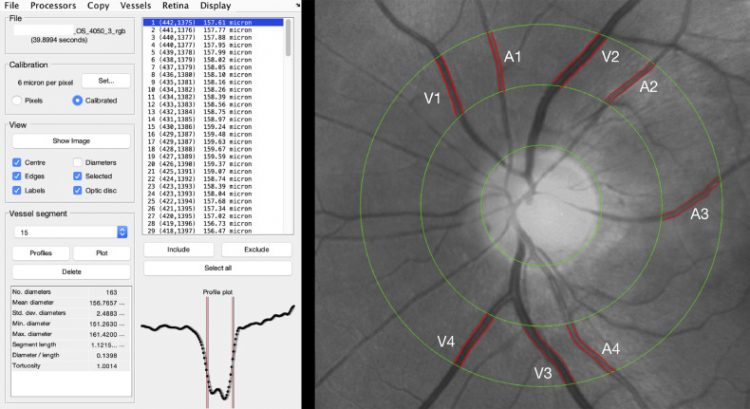
Fig. 1Retinal vessels analysis. The ARIA (automatic retinal image analyzer) software allowed to perform a semi-automatic assessment of retinal vessels diameter with an area of interest around the optic nerve area. For the purpose of the study, the main vessels within 0·5 and 1 disk diameter around the optic nerve head were automatically segmented by the software. The operator chose the four main veins and arteries and averaged their diameters automatically calculated by the software to obtain the mean arteries diameter (MAV) and the mean veins diameter (MVD), respectively.
For the purpose of the study we measured the diameter of the four main veins and the four main arteries comprised within the studied area and we obtained the mean artery diameter (MAD) and the mean veins diameter (MVD) by averaging the four arterial and venous values respectively.
Electronic charts of all patients were reviewed to collect demographic clinical and laboratory relevant parameters. The list included: age, sex, ethnicity, body mass index (BMI), smoking, alcohol consumption, presence of comorbidities (systemic hypertension, diabetes, dyslipidaemia, history of coronary disease/stroke, tuberculosis and HIV infection), COVID-19 related symptoms (cough, fever), time between the symptoms onset and the day of the fundus photography, systolic and diastolic blood pressure on the day of the fundus, oxygen support if needed (low flow oxygen, Venturi mask, continuous positive airway pressure), treatment received (anticoagulant, antiplatelet, hydroxychloroquine, remdesivir, lopinavir/ritonavir, tocilizumab, steroids). Treatments and comorbidities were considered as binary variables (YES/NO) without accounting for dosage or duration.
Laboratory parameters included haematocrit, white blood cells, neutrophils, lymphocytes and platelets count, prothrombin time (PT), partial thromboplastin time (PTT), Fibrinogen, D-Dimer, C reactive protein (CRP), ferritin, lactate dehydrogenase (LDH), creatinine, creatine kinase, and albumin tested within three days prior to fundus photograph collection.
Information regarding the age, sex, ethnicity, body mass index (BMI), smoking, alcohol consumption, presence of comorbidities (systemic hypertension, diabetes, dyslipidaemia, history of coronary disease/stroke, tuberculosis and HIV infection) were also collected in unexposed subjects. Comorbidities were considered as binary variables (YES/NO) without further characterization.
The primary outcome of the study was to assess the presence of alterations of the retina or the retinal vasculature in COVID-19 patients compared to unexposed subjects. The secondary outcomes were the association of demographic, clinical and laboratory parameters with retinal findings in the COVID-19 group.