Background
Financial incentives promote use of HIV services and might support adherence to the
sustained antiretroviral therapy (ART) necessary for viral suppression, but few studies
have assessed a biomarker of adherence or evaluated optimal implementation. We sought
to determine whether varying sized financial incentives for clinic attendance effected
viral suppression in patients starting ART in Tanzania.
Methods
in Shinyanga region, Tanzania, adults aged 18 years or older with HIV who had started
ART within the past 30 days were randomly assigned (1:1:1) using a tablet-based application
(stratified by site) to receive usual care (control group) or to receive a cash incentive
for monthly clinic attendance in one of two amounts: 10 000 Tanzanian Shillings (TZS;
about US$4·50) or 22 500 TZS (about $10·00). There were no formal exclusion criteria.
Participants were masked to the existence of two incentive sizes. Incentives were
provided for up to 6 months via mobile health technology (mHealth) that linked biometric
attendance monitoring to automated mobile payments. We evaluated the primary outcome
of retention in care with viral suppression (ClinicalTrials.gov,
NCT03351556.
Findings
Between April 24 and Dec 14, 2018, 530 participants were randomly assigned to an incentive
strategy (184 in the control group, 172 in the smaller incentive group, and 174 in
the larger incentive group). All participants were included in the primary intention-to-treat
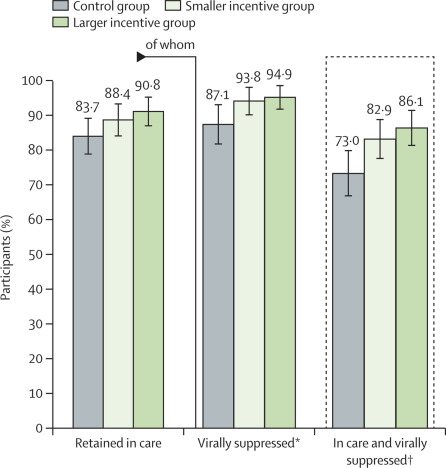
analysis. At 6 months, approximately 134 (73%) participants in the control group remained
in care and had viral suppression, compared with 143 (83%) in the smaller incentive
group (risk difference [RD] 9·8, 95% CI 1·2 to 18·5) and 150 (86%) in the larger incentive
group (RD 13·0, 4·5 to 21·5); we identified a positive trend between incentive size
and viral suppression (p trend=0·0032), although the incentive groups did not significantly
differ (RD 3·2, −4·6 to 11·0). Adverse events included seven (4%) deaths in the control
group and 11 (3%) deaths in the intervention groups, none related to study participation.
Interpretation
Small financial incentives delivered using mHealth can improve retention in care and
viral suppression in adults starting HIV treatment. Although further research should
investigate the durability of effects from short-term incentives, these findings strengthen
the evidence for implementing financial incentives within standard HIV care.
Funding
National Institute of Mental Health at the US National Institutes of Health.